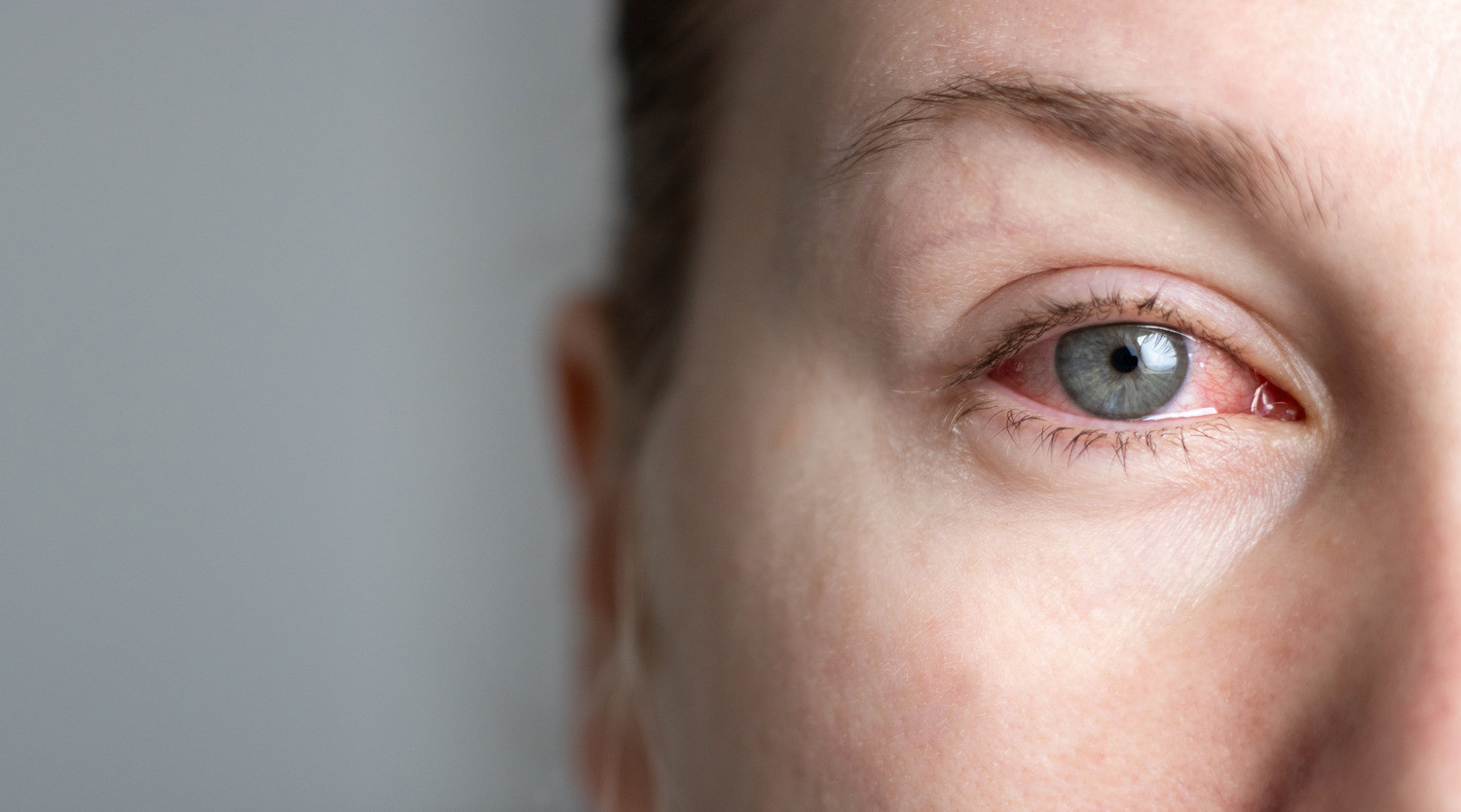
 Presentations of red eye related to medical procedures are expected to become more common in general practice, according to ophthalmologist Dr Xia Ni Wu.
Presentations of red eye related to medical procedures are expected to become more common in general practice, according to ophthalmologist Dr Xia Ni Wu.
Dr Wu, from South Street Ophthalmology, told Medical Forum it is an area that GPs will need to have a broader understanding of going forward.
This may be due to potential reactions to new drugs on the market that can affect the eyes and the increased administration of certain medications that are injected into the eye by ophthalmologists.
“There are some new medications on the market and increased potential for medication or procedural related red eye, so I think it’s going to be a bigger presentation in the future,” Dr Wu said.
“Dupilumab, which is being used for eczema, atopic dermatitis, and sometimes in asthma settings as well, can lead to dry eyes and red eye in its various forms.”
She said with dupilumab associated red eye an initial course of action for GPs to explore would be topical lubricants or drops.
In more severe cases, Dr Wu said immunotherapy related medications used for melanoma and other cancers can also lead to uveitis – a serious cause of red eye.
“In this case it’s about knowing when to call the eye registrar or call the local ophthalmologist. Tell them that the patient is on this medication and they’ve got red eye and decreased vision, do you mind seeing them?” she said.
RELATED: Keeping up with advances in laser eye surgery
Dr Wu said doctors will also have to be across the potential reactions to new injectable drugs on the market to treat dry macular degeneration. Ophthalmologists inject this medication into the eye.
“Every procedure has a risk and in this case the risk is infection which is sight threatening. If it’s someone after an injection and they’ve got problems, then it’s an urgent, same-day, call to the consultant or ophthalmologist,” she said.
Dr Wu said GPs could also assist in providing the best advice in terms of onward referral.
“It’s about knowing where to go. I’ve had patients to Fiona Stanley Hospital, they maybe three weeks post injection and they had to wait six or seven hours, only to be told that Fiona Stanley does not have an ophthalmology team on call.”
She said that “wasted time” can be avoided by making a few calls or asking questions.
Dr Wu will be speaking at Medical Forum Live, a clinical education event taking place on May 9 where attendees can earn up to 22 hours of CPD.
Her talk, Sorting the Serious from the Simple: Acute Red Eye for GPs will be one of the presentations taking place. The day will cover clinical education on common, acute and chronic presentations to general practice. Connect with colleagues from across WA and complete almost 50% of your yearly CPD requirements.
REGISTER TO ATTEND – SPACES ARE LIMITED
Want more news, clinicals, features and guest columns delivered straight to you? Subscribe for free to WA’s only independent magazine for medical practitioners.
Want to submit an article? Email [email protected]

